What Is Prostatectomy?
What Is Prostatectomy?

A prostatectomy is a surgical procedure to remove either part or all of the prostate gland, usually to treat localised prostate cancer or benign conditions in the prostate. Let’s take a look at the specifics of the procedure.
The term ‘prostatectomy’ is used to describe a number of different surgical procedures to remove either part or all of the prostate gland, which is found in the lower abdomen only in men.
The procedure is usually done to treat benign conditions in the prostate, or to treat localised prostate cancer and other pelvic cancers.
The prostate gland is a part of the male reproductive system. Its main role is to produce the fluid that carries and protects sperm.
Procedure
There are two main types of prostatectomy and a few sub-categories, depending on the treatment required.
Radical – Radical prostatectomy involves removing the entire prostate gland, capsule (or covering), the surrounding lymph nodes and neighbouring tissue. This is usually a treatment for men with localised prostate cancer and there a number of different common techniques used:
• Open radical prostatectomy – Where the prostate is removed via a single incision in the lower abdomen, or the perineum.
• Laparoscopic radical prostatectomy – Where the prostate is removed via several small incisions in the lower abdomen using special tools and techniques. This process is less invasive than open surgery.
• Robotic-assisted radical prostatectomy – Much like laparoscopic radical prostatectomy, the prostate is removed via small incisions in the lower abdomen. Robotic-assisted instruments are inserted through the incisions and controlled by a surgeon. This allows for far more precise movement of the surgeon’s hands meaning it is an even less invasive procedure overall.
Robotic-assisted surgery has multiple benefits over the traditional open operation including lower blood loss, reduced hospital stay as well as improved urinary control and erectile function after the operation.
Simple prostatectomy is when the enlarged prostate is removed by enucleating it from its capsule. The sphincter muscle and nerves remain intact. It is used to treat benign conditions such as enlargement of the prostate (benign prostatic hyperplasia or BPH).
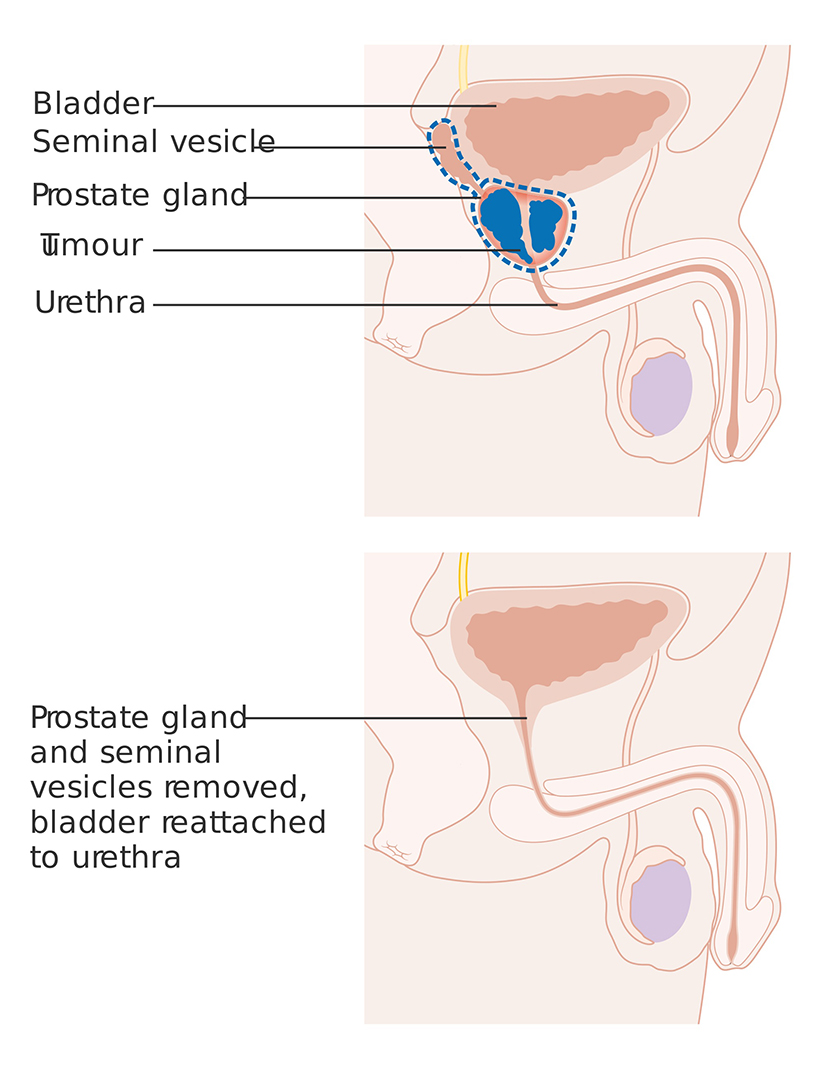
Risks and Side Effects
There are a few risks associated with the procedure, as with any major surgery. These include:
• Bleeding
• Infection
• Deep vein thrombosis
• Urinary tract infection (UTI)
Radical prostatectomy is a live-saving procedure, however there are some possible side effects. These include erectile dysfunction due to injury of the nerves surrounding the penis, urinary incontinence due to injury of the nerves or the urinary sphincter, or urinary obstruction (which is rare) where scar tissue forms at the point where the urethra is reconnected to the bladder. The transfusion rate is also very low.
Recovery
Following the procedure, patients are taken to recovery and monitored closely. Hospital stay is depend on multiple factors. At Nepean Public Hospital it is an overnight stay. At Macquarie University Hospital it is a two to three night stay. Dr Arianayagam usually keeps patients on fluids after surgery and then on normal food the next day.
Patients will have a urinary catheter in their bladder after surgery to drain urine. This will remain for about 1 week after surgery. There will be a drain tube as well that will be removed within a day or two of surgery, depending on the level of drainage. Patients will be taught how to take care of their catheter when they’re at home.
Once discharged from hospital, patients will need to take special care in order not to risk further injury or complications. The surgical area will need to remain dry and clean – specific bathing methods will be supplied by your doctor.
Full recovery might take up to six weeks. During this time, driving, heavy lifting and exercise is discouraged. You will be advised by your doctor when you can return to work.
Prostatectomy with Urology Specialist
We are experts in the field of prostatectomy. In particular, Dr Mohan Arianayagam specialises in robotic radical prostatectomy.
Dr Arianayagam performs robotic radical prostatectomy at both Macquarie University Hospital and Nepean Public Hospital. Dr Arianayagam has performed over 250 robotic cases. He is a proctor for Device Technologies, who supply the Da Vinci Robotic System in Australia. Being a proctor means Dr Arianayagam is qualified to teach other surgeons to use this technique.
If you have any questions regarding prostatectomy, laparoscopy or would like to book an appointment, please feel free to contact Urology Specialist here.

Why Does Testicular Pain Persist? Common Causes to Know
Testicular pain is relatively common; however, when it becomes severe and long-lasting, there may be some cause for concern. This…

Everything You Need to Know About Sperm Health
It is not uncommon for men to have troubles with their sperm production, or to develop a sperm disorder. But…