What are the Different Types of Prostate Surgery?
What are the Different Types of Prostate Surgery?

Surgery may be required to treat a range of conditions that affect the prostate. Here we take a look at the three most common types of prostate surgery.
Prostate surgery is a very effective treatment for a number of conditions, the two most common being prostate cancer and benign prostatic hypertrophy (BPH – also known as an enlarged prostate).
In the case of cancer, these procedures are performed to stop the spread of malignant cells. For BPH, surgery may be required to relieve symptoms that are making it difficult to urinate, which can have a significant impact on quality of life.
What is The Prostate?
The prostate gland is a part of the male reproductive system. Its main role is to produce semen, the fluid that carries and protects sperm. It is about the size of a walnut and sits just below the bladder in men.
The prostate is surrounded by the upper part of the urethra, the thin tube that carries urine from the bladder to the penis. It also carries semen from the prostate and sperm from the testicles to penis during ejaculation.
The Different Types of Prostate Surgery
Prostatectomy
The term ‘prostatectomy’ is used to describe a number of different surgical procedures to remove either part or all of the prostate gland. This may be required to treat prostate cancer or BPH.
When only a part of the prostate is removed, this is called a simple prostatectomy. This process involves enucleating it from its capsule to trim away excess tissue, but where the sphincter muscle and nerves remain intact. It is usually used to treat BPH, which is a benign condition, meaning there is no risk of malignant cells having moved on to surrounding tissue.
When the entire prostate gland, capsule (or covering), the surrounding lymph nodes and neighbouring tissue is removed, this is known as a radical prostatectomy. This is usually a treatment for men with localised prostate cancer and there a number of techniques used:
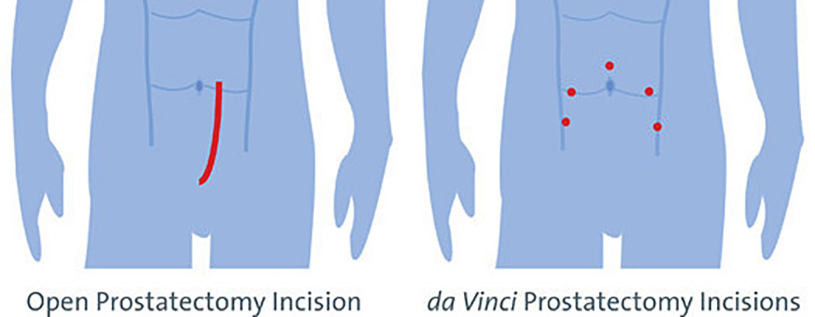
Open Surgery – This is where the prostate is removed via a large single incision in the lower abdomen, or the perineum (the spot between the anus and the testicles).
Laparoscopic Radical Prostatectomy – This is where the prostate is removed via several small incisions in the lower abdomen using small surgical instruments. This process is much less invasive than open surgery.
Robotic-assisted radical prostatectomy – Much like laparoscopic radical prostatectomy, the prostate is removed via small incisions in the lower abdomen. Robotic-assisted instruments are inserted through the incisions and controlled by a surgeon.
This allows for very precise movements, meaning it is an even less invasive procedure overall. This has multiple benefits over open surgery, including lower blood loss, reduced hospital stay, and improved urinary control and erectile function after the operation.
Holmium Laser Enucleation of the Prostate (HoLEP)
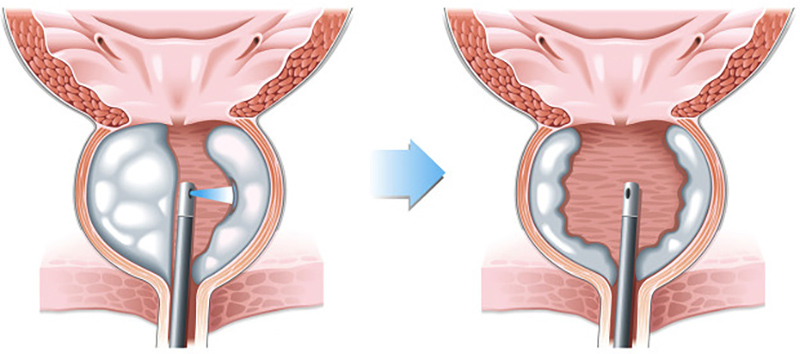
Holmium laser enucleation of the prostate – abbreviated as HoLEP, or laser prostate surgery – is another minimally invasive surgery. It is used to treat symptoms of BPH by removing blockages to urine flow.
This is achieved by inserting an instrument called a resectoscope into the urethra to get a visual of the prostate tissue and the lining of the bladder. Then a laser is used to cut away the obstructing tissue. An instrument called a morcellator is the used to cut the resected prostate tissue into smaller pieces. The tissue is then removed via the rectoscope.
Laser surgery is an effective way to operate on symptoms quickly and efficiently, and the procedure greatly reduces recovery time and postoperative complications.
Transurethral Resection of the Prostate
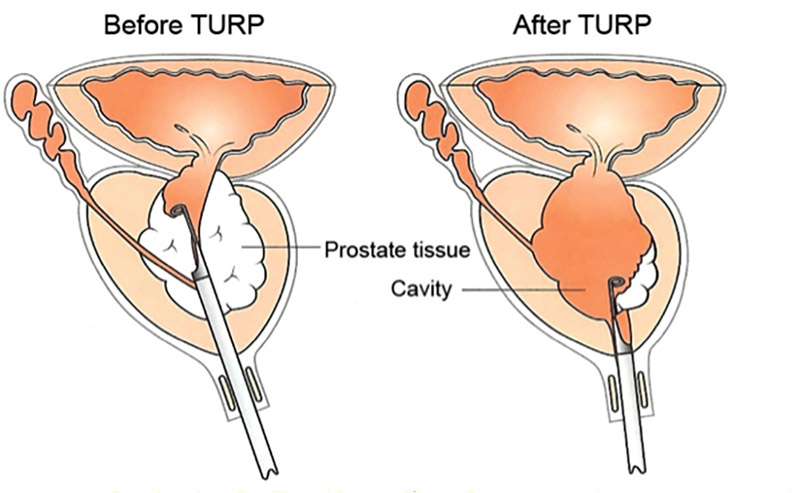
A transurethral resection of the prostate – abbreviated as TURP – is another operation to treat symptoms of BPH by removing blockages to urine flow.
Rather than using a laser, the procedure employs a resectoscope into the urethra to get a visual of the prostate tissue and the lining of the bladder. Using the resectoscope, the urologist is able to trim away enlarged lobes of the prostate. The capsule of the prostate is left intact.
Common Side Effects of Prostate Surgery
There are three main complications associated with prostate surgery: urinary problems, erectile dysfunction and sexual dysfunction.
Urinary problems may be where you have trouble holding in urine, urination may be painful or you may have difficulty going to the bathroom, or you may frequently experience the sudden need to urinate (urge incontinence). These side effects are normal and usually take a few weeks to subside. Long-term effects are quite rare.
Erectile dysfunction is common following surgery. Function usually returns within 8-12 weeks. Long-term ED is possible, however, minimally invasive surgery such as laparoscopic or robotic laparoscopic surgery minimises the chance of it occurring.
Most patients will not ejaculate properly after prostate surgery, and this is irreversible. This is because the semen glands are removed during the operation. Hence, it is not recommended for younger men.
Prostate Surgery with Urology Specialist
Dr Arianayagam is highly experienced in all aspects of prostate surgery, in particular robotic radical prostatectomy.
Dr Arianayagam performs robotic radical prostatectomy at both Macquarie University Hospital and Nepean Public Hospital. Dr Arianayagam has performed over 250 robotic cases. He is a proctor for Device Technologies, who supply the Da Vinci Robotic System in Australia. Being a proctor means Dr Arianayagam is qualified to teach other surgeons to use this technique.
If you have any questions regarding prostate surgery, or would like to book an appointment, please feel free to contact Urology Specialist here.

Everything You Need to Know About Sperm Health
It is not uncommon for men to have troubles with their sperm production, or to develop a sperm disorder. But…

The Benefits of Drinking Water for Urological Health: Do You Really Need 8 Glasses a Day?
We’ve all heard the advice: “Drink eight glasses of water a day” But is this rule as important as it…