Nephrectomy is a surgical procedure to remove either part or all of the kidney, usually to treat cancer and other kidney diseases. Let’s take a look at the specifics of the procedure.
Nephrectomy is a surgical procedure to remove either part or all of the kidney. The kidneys are vital organs that filter water and other waste products from your blood, produce urine and hormones, and maintain levels of minerals in your bloodstream. They are small and bean-shaped, and are located in the upper back of the abdomen.
Nephrectomy is usually carried out in order to treat cancer and other kidney diseases, to remove an organ that is damaged or to remove a healthy kidney for transplantation.
There are two main types of nephrectomy:
Radical – Radical nephrectomy involves removing the whole kidney, along with a section of the tube leading to the bladder called the ureter, the adrenal gland which sits atop the kidney, and the fatty tissue surrounding the kidney. If both kidneys need to be removed, this is called bilateral nephrectomy.
Partial – For a partial nephrectomy, only the diseased or injured portion of the kidney is removed.
Procedure
Nephrectomy is performed with the patient under general anaesthesia. The procedure is executed either as open surgery, laparoscopically or as robotic surgery.
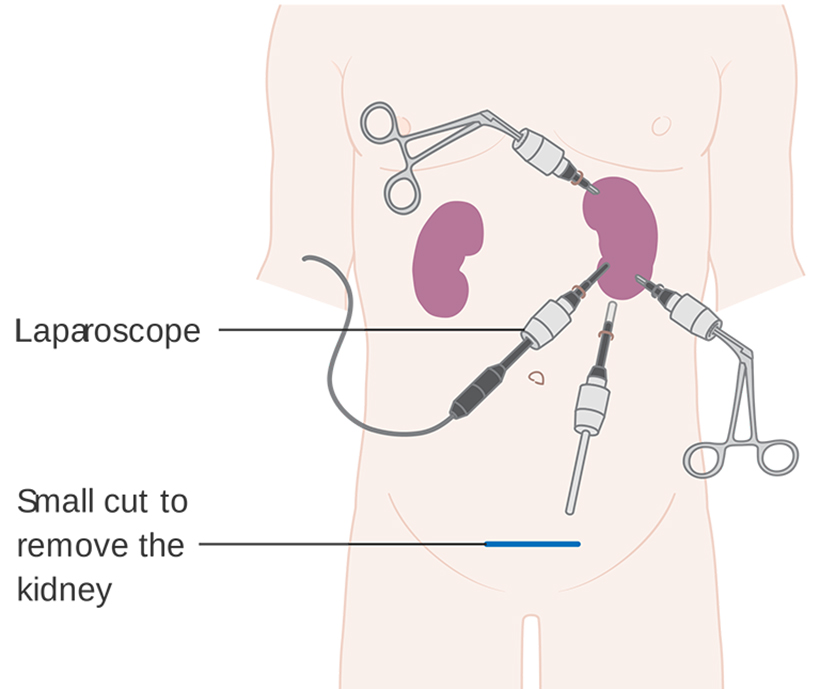
Laparoscopy uses three or four small abdominal incisions and fibre-optic technology to operate and is far less invasive than open surgery; as such, the recovery time is much quicker. The kidney is detached internally, placed in a bag, then removed through one of the incisions.
For open nephrectomies, an incision is made in the side of the abdomen and sometimes, depending on the circumstances, also in the midline. Sometimes a rib may need to be removed to perform the procedure. The ureter and the surrounding blood vessels are detached and the kidney is removed via the incision. The opening is then closed with stitches.
Risks and Side Effects
There are a few risks associated with nephrectomy, though serious complications are uncommon:
• Loss of blood
• Heart attack or stroke
• Allergic reaction to anaesthesia or medication
• Pulmonary embolism – the formation of a blood clot in your legs that may move into the lungs
• Infection at the site of the incisions
• Postoperative pneumonia
• Injury to organs or tissue around the kidney
• Problems with remaining kidney
• Kidney failure
Potential long-term side effects of kidney removal are often associated with the loss of full kidney function (with both organs). This may result in high blood pressure (hypertension) or chronic kidney function.

Recovery
Recovery after nephrectomy is contingent on the patient’s overall health and the type of procedure performed.
Immediately after surgery, patients are monitored for blood pressure, electrolyte levels and fluid balance i.e. the bodily functions performed by the kidney. Patients will often have a urinary catheter in their bladder for a short time after surgery to drain urine.
Pain and numbness at the incision site is common for a period after the surgery. Coughing or sneezing is usually quite painful due to the proximity of the kidneys to the diaphragm, however, deep breathing exercises are strongly recommended following nephrectomy in order to prevent postoperative pneumonia.
Recovery times will be different for each patient and the procedure. Patients who have had laparoscopic surgery will usually stay in hospital for 2-3 nights while those who have had open surgery stay for 5-7 nights. Heavy lifting and other strenuous activities are discouraged for up to 6 weeks and driving is discouraged for up to 2 weeks. However, light activities are recommended whenever the patient feels up to it.
Information on diet and exercise regimes are usually given to patients before they leave hospital.
Nephrectomy with Urology Specialist
We are experts in the field of nephrectomy. In particular, Dr Mohan Arianayagam specialises in laparoscopic partial nephrectomy where a diseased portion of the kidney is removed leaving the rest of the organ intact.
He also performs zero ischaemia partial nephrectomy, where the artery to the kidney is not clamped. This has the advantage of having no ischaemia to the kidney and hence improved function. It is even more challenging than the traditional laparoscopic approach due to the risk of increased bleeding. Results of this technique was presented at the recent Urological Society of Australia and New Zealand in 2014.
If you have any questions regarding prostatectomy or would like to book an appointment, please feel free to contact Urology Specialist here.

