What Is a Vasectomy?
What Is a Vasectomy?
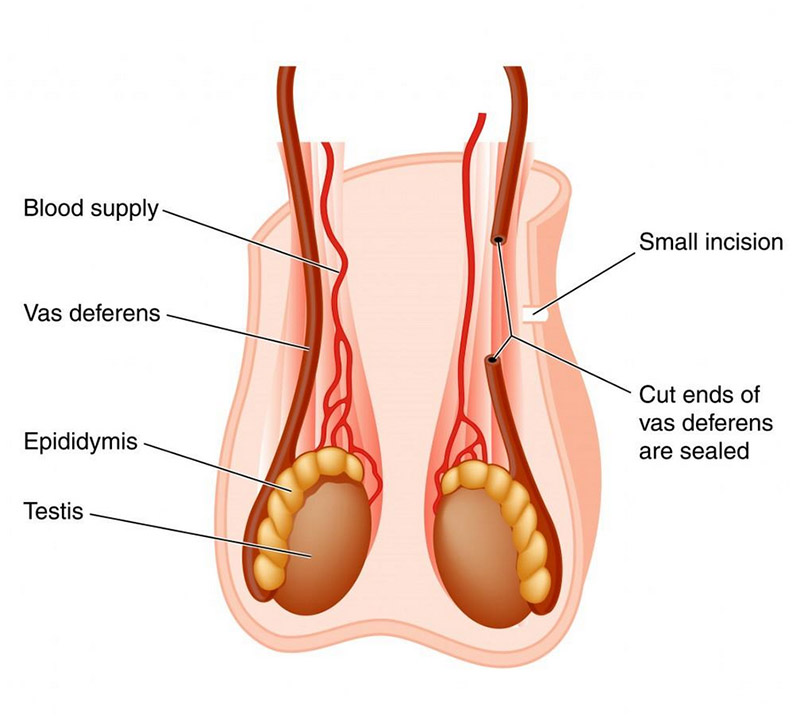
Vasectomy is a surgical procedure for permanent contraception in men that involves cutting both the tubes that carry sperm from the testicles to the penis.
Vasectomy is a common surgical procedure for permanent contraception in men. Its method involves cutting and blocking the vas deferens – a tube located in the groin that carries sperm from the testicles to the penis.
The vas deferens is a muscular tube roughly 30cm long. It acts as a passage between the epididymis (a coiled tube located at the back of each testicle) and the prostate where semen is ejaculated from during sexual climax. From the prostate the semen is then ejaculated out of the penis via the urethra.
Only about 2% of the semen comes from the testicles via the epididymis and vas deferens, but this percentage contains all of the sperm necessary for impregnation. Therefore, when the vas deferens is cut, the volume of fluid ejaculated is roughly the same, however, it contains none of the vital sperm.
Vasectomies are quite common in Australia with over 25,000 men opting for the contraceptive procedure each year. Roughly 1 in 4 men over the age of 40 have had a vasectomy.
Procedure
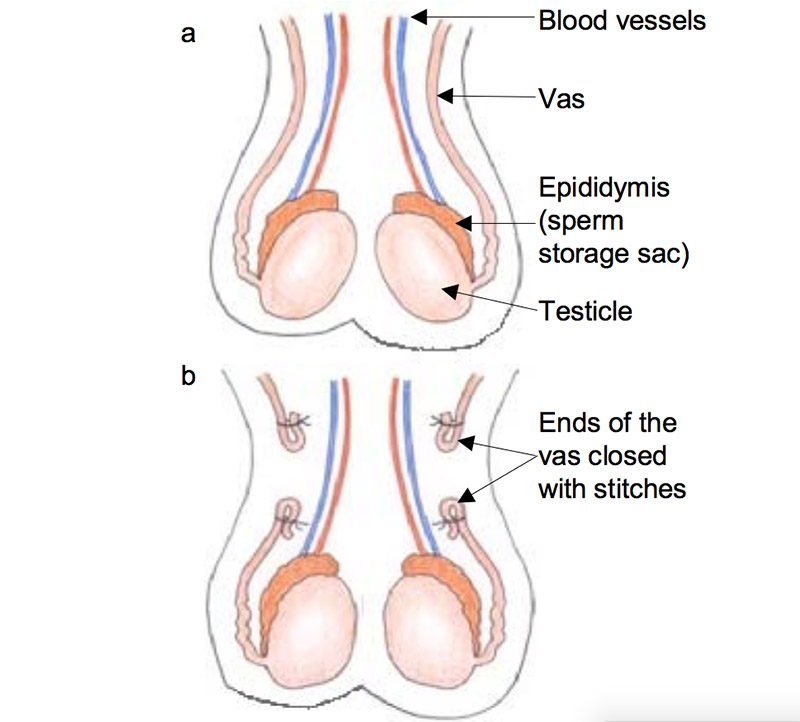
Vasectomy is a relatively simple procedure. Patients are given general anaesthetic. The urologist then makes two small incisions in the scrotum. Through these openings the two vas deferens are cut and a small piece is removed.
The ends of the vas deferens are then tied, stitched or sealed (diathermy is commonly used to seal the ends using heat). The scrotum is then stitched up. The whole procedure takes 15-30 minutes.
Recovery Time
After surgery, the scrotum is often numb for 1-2 hours. Bruising, mild pain and discomfort is common for a few days. Wearing supportive underwear can help reduce discomfort. Patients can usually return to work after a few days (unless the work is particularly strenuous). Heavy lifting is discouraged for up to a week.
If the patient feels up to it, sexual intercourse can be resumed after a week. However, it can take a few months for sperm to completely clear out. Semen analysis is required 2-3 months after surgery to ensure the sperm count is at zero. Until this is confirmed, alternative methods of birth control are necessary. If the sperm count is not at zero, further testing is required every month until it is confirmed there is no live sperm in the semen.
A vasectomy will not affect sex drive, ability to achieve sexual climax or ejaculate, or the ability to have erections. Mild discomfort in the testicles during intercourse is common in the months following a vasectomy.
Risks and Side Effects
As with any type of surgery, there are a few risks associated with vasectomy, including bleeding and infection. Long-term pain and discomfort in the testicles is also possible and some men may experience pain during ejaculation.
There is also the possibility of sperm leaking from the vas deferens and forming a small lump in the tissue around it (called a sperm granuloma). Inflammation of the epididymis is also possibility.
In very rare cases, ‘recanalisation’ may occur. This is where vas deferens reconnects, allowing sperm to pass from the epididymis to mix with the semen.
Vasectomy with Urology Specialist
While he is primarily a urological cancer surgeon, Dr Arianayagam also sees patients with more general urological problems. Dr Arianayagam performs several vasectomies each month, usually at the Hospital for Specialist Surgery in Bella Vista.
You can refer to this sheet more information on vasectomy, or if you have any further questions or would like to book an appointment with a urologist in Sydney, please feel free to call.

Protect Your Kidneys: Simple Habits for Better Health
Keeping your kidneys in shape is vital for reducing the risk of chronic disease. Check out some of our top…

Boost Your Urological Health with the Help of Technology
Check out some of the different technological tools you can adopt to care for your urological health. While we all…